
An established transcription factor known for bone formation also supports specialized cells in the central nervous system to promote brain tissue stiffness, findings that could inform new therapeutics for neuronal regeneration, according to a Northwestern Medicine study published in Neuron.
“We have uncovered the molecular mechanisms that control extracellular matrix production by oligodendrocytes that, interestingly, includes the same regulatory molecule that controls bone formation. Whenever this regulation is disrupted, oligodendrocytes do not function properly, which leads to a disruption in neuronal function,” said Brian Popko, PhD, the William Frederick Windle Professor of Neurology and co-corresponding author of the study.
Oligodendrocytes are a specialized type of central nervous system (CNS) cells called glial cells, which support communication between neurons. The main function of oligodendrocytes is to produce myelin, which surrounds axons (nerve fibers) in an insulating sheath to help nerve signals properly travel throughout the CNS.
Recent work suggests that oligodendrocytes also provide metabolic support to neurons and support a wide range of brain functions as well as being involved in different neurodegenerative diseases. These cells also produce key components of the CNS’s extracellular matrix (ECM), which is composed of large molecules that surrounds cells of all tissues and organs, providing structural support, as well as support for myriad cellular functions.
In the current study, the investigators aimed to characterize which transcription factors control ECM-related gene expression in oligodendrocytes.
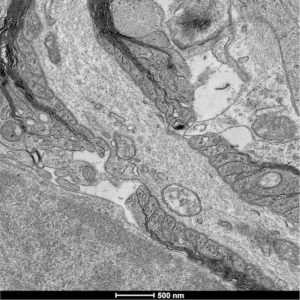
“The role of oligodendrocytes in generation of the extracellular matrix and in establishing the bio-mechanical properties of the brain is overlooked and was currently unknown,” said Benayahu Elbaz-eilon, PhD, assistant professor in the Ken and Ruth Davee Department of Neurology Division of Multiple Sclerosis and Neuroimmunology and co-corresponding author of the study.
Using a combination of atomic force microscopy and genetic and transcriptional study techniques, the investigators explored how oligodendrocytes contribute to CNS stiffness, which plays a fundamental role in nearly all biological processes in the brain, including development, regeneration and aging, according to Elbaz-eilon.
“Establishing accurate CNS biomechanics is an important but largely overlooked function of oligodendrocytes,” Elbaz-eilon said.
Using these techniques, they discovered that Osterix, an established transcription factor in bone formation, binds to genes in oligodendrocytes essential for ECM function and gene expression related to nodes of Ranvier, or small gaps in myelin sheaths. Osterix has been shown to control the maturation of osteoblasts, which are essential for promoting bone formation and growth.
The findings suggest Osterix is required in oligodendrocytes for the development, maintenance and regeneration of myelin in the CNS and supports brain and bone tissue stiffness.

“Many neurological disorders include the loss of oligodendrocytes. This, of course, disrupts CNS myelination, but it also changes the ECM composition of the brain. We are just beginning to understand the implications of an altered ECM in the functioning, repair and aging of the nervous system,” Popko said.
The investigators are now interested in characterizing ECM composition and brain stiffness inside and near focal lesions in the brain. They also aim to identify new therapeutic targets that will help transform the ECM around brain lesions into a microenvironment that promotes neural and myelin regeneration.
“The scientific community is constantly looking for new ways to promote brain regeneration and formatting of new myelin, instead of the myelin that was lost in disease. The ability of the brain to regenerate depends in many ways on brain stiffness. Full understanding of the molecular pathways that control brain stiffness in health and disease will enable us to harness these findings for finding new therapeutic options,” Elbaz-eilon said.
This work was supported by National Institutes of Health grants R01NS067550, R01NS109372, R01NS099334, 1RF1AG072080, and R35NS132349; the National Multiple Sclerosis Society (RG-1807-32005) grant; the Dr. Miriam and Sheldon G. Adelson Medical Research Foundation and the Rampy MS Research Foundation; Department of Defense grant W81XWH2210386; the British Council GROWTH fellowship; the Dr. Willem Been Legacy award; and Israel Cancer Research Fund grant 01301.






