Investigators from the laboratory of Alicia Guemez-Gamboa, PhD, assistant professor of Neuroscience, have discovered new molecular mechanisms of PACS1 syndrome, a rare neurodevelopmental disorder, according to findings published in Nature Communications.
PACS1 syndrome is characterized by intellectual disability and distinct craniofacial abnormalities. Patients may also experience epilepsy, autism, hypotonia (muscle weakness), feeding difficulties, and heart defects. The disorder, which was first identified in 2012, is caused by a single sporadic variant in the PACS1 (phosphofurin acidic cluster sorting 1) gene.

“Most neurodevelopmental disorders result from many different variants, but with PACS1 syndrome all patients have the same one, so it’s a pretty unique situation,” said Lauren Rylaarsdam, PhD, a former graduate student in the Guemez-Gamboa laboratory and lead author of the study.
There are approximately 200 known cases of PACS1 syndrome, most of which have been reported in children, although recent advances in genetic sequencing technology may help identify more patients.
“Unfortunately, there are no therapies available, so we teamed up with the PACS1 Syndrome Research Foundation to try and figure out how the variant impacted the developing brain and how to fix it,” Guemez-Gamboa said.
To do this, the authors obtained stem cells reprogrammed from patient skin fibroblasts — cells that help form connective tissue — and also used gene editing tools to introduce the PACS1 syndrome-causing variant into healthy cells and correct it in patient cell lines. The authors then differentiated these cells into neurons to understand how the PACS1 variant impacted the developing brain.
Because little was previously known about PACS1 syndrome, the scientists used a variety of tools, including single-cell RNA sequencing of cerebral organoids — a cutting-edge 3D culturing technique in which many different neural cell types grow simultaneously in small spheres.
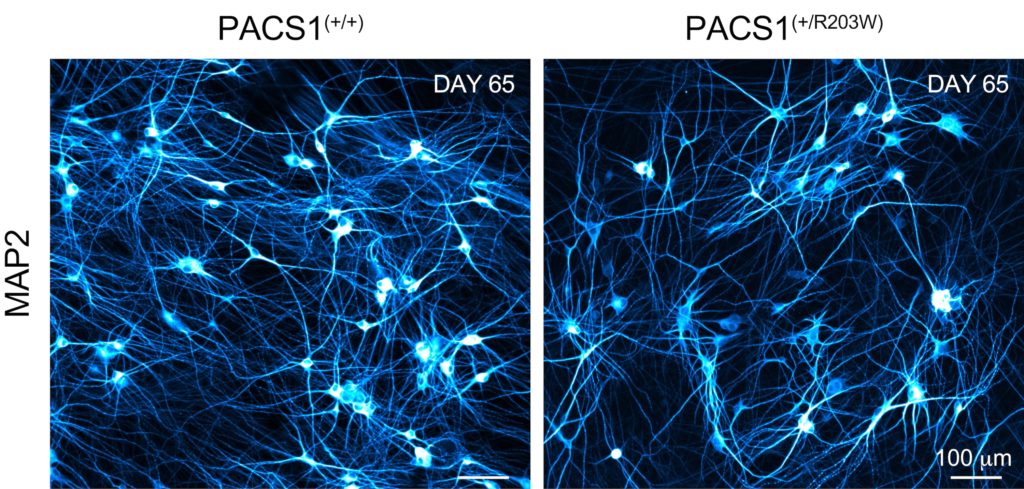
Interestingly, they found that mature excitatory neurons appeared more affected than young excitatory neurons. Mature neurons in PACS1 syndrome organoids also had impaired expression of genes related to synaptic signaling – the primary method of communication between neurons in the brain.
“This, in conjunction with the epilepsy and autism that patients experience, led us to think that there could be some differences in the firing patterns of PACS1 syndrome neurons,” Rylaarsdam said.
The investigators then captured the activity of PACS1 syndrome excitatory neurons using multielectrode arrays, which allowed them to record the activity of many cells at once. Using this technique, the scientists discovered that bursts of activity lasted much longer in neurons containing the PACS1 variant.

“This is a huge step towards beginning to understand what might contribute to the epilepsy and autism that patients experience,” Rylaarsdam said.
Moving forward, the investigators said they plan to determine if neurons are similarly affected in mouse models of PACS1 syndrome. Their ultimate goal, according to Rylaarsdam, is to identify and test therapies that repair the phenotype observed in neurons with the PACS1 mutation.
“The brain is composed of many diverse regions connected by an intricate circuit system, so it is important to understand how the increase in burst duration I saw in a very isolated context correlates to the brain as a whole. We found some preliminary evidence to suggest that the inhibitory neurons of the brain are also affected, but our models were better suited to study excitatory neurons, so that’s also an area where the mouse model will be really important,” Rylaarsdam said.
This work was funded by the PACS1 Syndrome Research Foundation and National Institutes of Health grant R01NS123163.






