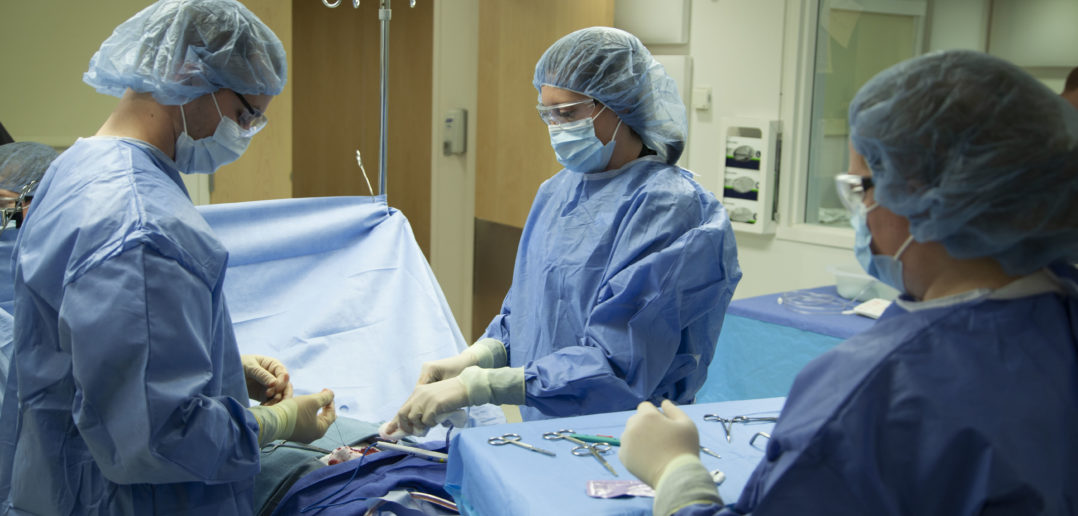
In the lower level of McGaw Pavilion, visitors are greeted by a pair of sliding glass doors leading to what looks exactly like a functioning hospital. To the untrained eye, it’s easy to think it is one — and that’s exactly the goal of Northwestern Simulation.
Since 2010, Northwestern Simulation has provided medical students, residents, trainees, fellows, practicing clinicians and ancillary teams at Northwestern and around the world a safe learning space to practice and improve their skills through simulation-based learning without the pressure of a real clinical setting — or potentially putting patients at risk.
Those who utilize the center are from the Northwestern community, as well as from various medical societies, government organizations and industry leaders in healthcare, science, engineering and technology.
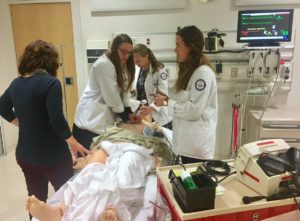
To ensure the center’s smooth day-to-day function and accessibility, a team of experts are responsible for creating an environment at the center that is welcoming and fully equipped for the specific needs of whoever steps inside.
“Ultimately, Northwestern Simulation is about improving patient care, giving aspiring and current healthcare providers and leaders the opportunity to hone their skills and reach levels of proficiency – or mastery – before applying those skills and procedures in a real clinical setting,” said Eric Hungness, MD, director of Northwestern Simulation and the S. David Stulberg, MD, Professor of Advanced Surgical Education.
Hungness leads a large group of scientists at Northwestern Simulation and has won several awards for his work in the center. For example, Hungness and Ezra Teitelbaum, MD, MEd, assistant professor of Gastrointestinal Surgery, are continuing to push forward the Laparoscopic Common Bile Duct Exploration project. The now commercially available simulator and Mastery Learning curriculum, which were both developed at the Simulation Center, was recently featured for the fourth consecutive year at the American College of Surgeons (ACS) Hands-on Rural Surgery Skills course. Data from the three preceding courses was presented by sixth-year general surgery resident Ryan Campagna at this year’s ACS Surgical Forum and won the 2019 Excellence in Research Award for Surgical Education.
Northwestern Simulation provides the freedom for students and professionals alike to actively learn technical, procedural and communication skills while making mistakes. According to Hungness’ research, skills gained in the lab have been translated to the bedside at Northwestern Memorial hospital, leading to improved patient outcomes and a reduction in medical errors, hospital length of stay and patient costs.
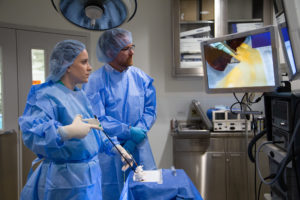
The space is comprised of mock surgical suites, patient examination rooms and a virtual reality lab designated for practicing intricate surgical procedures, all of which are equipped according to the needs of the specific training being performed. Mannequins and standardized patients (paid actors) available at the center provide the opportunity for students, residents and trainees alike to actively manage patients, practice procedures and provide care. In turn, the fear and risk of patient harm and medical errors is significantly reduced.
“Simulation is an incredible learning environment because it allows students to actively integrate and apply concepts learned in the classroom,” said David Salzman, MD, MEd, director of simulation for undergraduate medical education and an associate professor of Emergency Medicine and Medical Education.
The simulation lab is a hub for active learning, Salzman said, where students are able to integrate physical exam findings into practice, such as recognizing the physiologic mechanisms accounting for a specific disease process to initiating treatment and observing if treatment strategies produce desired outcomes.
“Unlike caring for patients in the clinical environment, where an error in medical judgement or initiation of an incorrect patient care practice can carry significant risk to the health and well-being of the patient, in the simulation center those errors are simply opportunities for discussion and learning to minimize the chances of the same error occurring when patient’s lives are at risk,” Salzman said.
For third-year medical student Jonathan Alhalel, Northwestern Simulation has allowed for a smoother transition into healthcare teams by having the opportunity throughout his medical school career to practice clinical skills — such as interpreting patients’ symptoms, monitors, and identifying appropriate conditions to administer oxygen therapy to patients — in a low-pressure setting.

“During the first two years of medical school when students don’t have as much exposure to the clinical world, the ability to transfer acquired textbook knowledge to a real scenario does wonders for how students approach each condition in the future,” Alhalel said.
For medical students, aspects of simulation are introduced as early as their first year, and by their third year, they learn basic skills such as IV placement, simple suturing, nasogastric tube insertion, urinary catheter insertion and sterile technique for gowning and gloving for the operating room. Standardized patients who have known anatomic or physiologic abnormalities or disease processes that students must examine and discover are also recruited to bring learning and testing to an even more realistic level.
Once senior students have determined their desired career path, they have the opportunity to participate in simulation “boot camps” at the center prior to graduation to prepare them for surgical residency. There they learn more advanced diagnostic techniques and skills such as advanced cardiac life support, ultrasound, trauma evaluation, central venous access and advanced suturing.
“I cannot speak highly enough about the Northwestern Simulation Lab. The folks that work here are incredibly dedicated and work very hard to set up labs and have everything run smoothly,” said Amy Holmstrom, MD, a general surgery resident.
Holmstrom is also a research resident and, having an office positioned in the simulation center, knows it is always busy with other residents, fellows, medical students and even high school students practicing their skills with simulators available at all hours.
For Holmstrom and other general surgery residents, each year builds on itself. The first year focuses on basic surgical skills like central line and chest tube insertion and advances in complexity in the second and third year to vascular and bowel anastomosis. Each year also includes verification of proficiency with summative evaluations to ensure that all residents have reached a minimal passing standard.
Finally, in the fourth and fifth years, entire surgical procedures are simulated on a variety of tissue models and residents are required to pass two skills exams prior to graduating: Fundamentals of Laparoscopic Surgery and Fundamentals of Endoscopic Surgery.
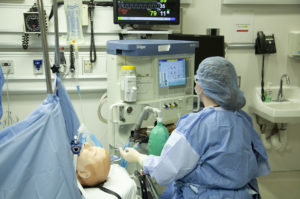
Recently, Northwestern Simulation was reaccredited as a Comprehensive Education Institute by the American College of Surgeons (ACS) through June 30, 2024. To be reaccredited an ACS Accredited Education Institute (ACS-AEI), institutes and skills centers must undergo a rigorous application and evaluation process to ensure all phases of surgical education and training meet ACS-AEI Standards and Criteria.
Additionally, the lab’s curriculum development and resources for delivery of effective education to faculty annually — such as simulation educator training workshops, faculty development sessions and train the trainer events — were identified by the ACS as areas of “best practice”.
“After review by the Accreditation Review Committee, multiple best practices were identified with no areas of partial or non-compliance,” according to the reaccreditation report. “Northwestern has maintained its strong track record of delivering effective education in simulation, and we look forward to your ongoing contributions to the Consortium and to the field of simulation-based surgical education and training.”






