
A new Northwestern Medicine study provides an explanation for how mutations in a sodium channel lead to a genetic disorder featuring insensitivity to pain. The findings, published in The Journal of Clinical Investigation, could also have implications for the development of novel anti-pain drugs.
In particular, the research illuminated how gain-of-function mutations in the sodium channel NaV1.9 are capable of turning off pain-sensing neurons completely or, conversely, heightening their sensitivity and causing them to fire even when unprovoked.
“We now understand this paradox of gain-of-function in NaV1.9 causing both loss of pain and gain of pain. This was a very confusing problem in the field, which we now have solved,” said principal investigator Alfred George, Jr., MD, chair and Magerstadt Professor of Pharmacology.
Carlos Vanoye, PhD, research associate professor of Pharmacology, was the co-first author of the study, which was conducted in collaboration with investigators at Yale University School of Medicine.
NaV1.9 is one of three voltage-gated sodium channels, along with NaV1.7 and NaV1.8, known to be important for pain sensation in the peripheral nervous system. Mutations in the genes encoding these sodium channels have also been tied to a number of genetic pain disorders, ranging from a condition where patients are unable to feel pain entirely to another disorder causing sudden, severe attacks of pain.
As such, there has been significant interest in investigating the genetics behind these pain disorders, which may validate targets for novel pain therapies.
“Mutations had been identified in NaV1.9 in families that had no pain sensation from birth,” explained George, also director of the Center for Pharmacogenomics. “So we started investigating the functional consequences of those mutations and imagined that we might learn how a drug should modify the channel to alleviate pain.”
George and his collaborators have been particularly focused on NaV1.9, as the sodium channel seemed to lend itself to more selective targeting, compared to NaV1.7 and NaV1.8.
But while previous research on NaV1.7 and NaV1.8 had established a clear relationship between gain-of-function in the channel causing severe pain, and loss-of-function leading to insensitivity to pain, the mechanisms behind NaV1.9 were more complex: Gain-of-function mutations in the channel appeared to cause both loss of pain perception and severe attacks of pain.
“This made no sense — clearly, just knowing what the mutation does to the sodium channel wasn’t the whole story,” George said. To investigate the question, his lab teamed up with scientists at Yale to understand the effect of the mutations on actual nerve cells.
The explanation, they discovered, is that there are different degrees of a gain-of-function in the sodium channel: A mild gain-of-function heightens pain sensation, while a more extreme gain-of-function eliminates pain perception.
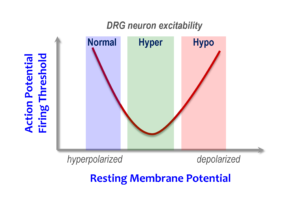
“A small perturbation in membrane voltage — which is what happens with a minor gain-of-function — will lower the amount of electrical current needed to fire a neuron. So it’s easier to trigger signaling in pain neurons,” George explained. “But a severe gain-of-function in the sodium channel will depolarize (e.g., make less negative) the neuron severely, and get to a state where it can’t fire an impulse.”
The findings, beyond leading to a deeper molecular understanding of the two genetic disorders, could also inform future drug discovery in targeting NaV1.9.
“Drugs could be developed to modulate NaV1.9 activity and then tested for analgesic effects,” Vanoye explained.
Additionally, while the scientists initially believed that understanding how the sodium channel behaved would provide a blueprint for how to build a novel drug to block pain, the study’s findings suggest a need to rethink the strategy.
“A drug that exactly mimics the effect of the natural mutation might be difficult to fine-tune as an analgesic, because of the chance of having a partial effect and thus changing the channel in the way that would actually increase pain,” George said. “The result from this study has really changed how we think about NaV1.9.”
George is also a member of the Robert H. Lurie Comprehensive Cancer Center of Northwestern University and the Center for Genetic Medicine.
The study was supported by National Institutes of Health grant NS032387; the Northwestern Medicine Catalyst Fund; the Rehabilitation Research and Development Service and Medical Research Service of the Department of Veterans Affairs; and the Erythromelalgia Association.






