Hyewon Phee, PhD, assistant professor in Microbiology-Immunology, studies the development of T-cells, a type of immune cell produced in the thymus. Although many mechanisms have been identified in the creation of T-cells, many details remain unknown.
“Within the thymus development of healthy T-cells occurs. When the T-cells have matured, they leave the thymus and circulate in the blood,” said Phee. “T-cells are important because they are programmed to look for various pathogens such as those found in viral and bacterial infections.”
Phee found a signaling pathway that may lead to T-cell immunodeficiency. The findings were published recently in eLife. T-cell immunodeficiency diseases can be hereditary, such as bubble baby disease, also known as severe combined immunodeficiency, or acquired, such as in AIDS and cancer chemotherapy.

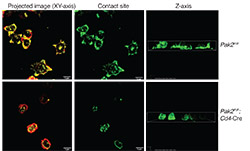
Phee identified a group of proteins that are important in the development of T-cells called p21-activated kinases (Pak2). She developed a novel mouse model where the gene for Pak2 was only deleted in T-cells, making it possible to test how the protein affects T-cells.
What she found was that the mouse models had significantly lower levels of T-cells than healthy mice. Further, the absence of Pak2 in thymocytes – the cells that become T-cells – prevented them from developing and producing a receptor protein that is necessary for the T-cells to leave the thymus and enter the blood.
“There are still many unanswered questions on how T-cells mature, but our paper suggests that Pak2 plays an important role in their development. We think our findings can provide some mechanistic insight in how immune deficiency disease can occur,” she said.
The research was funded by grants from the National Institutes of Health 5K01AR059754.






