
Precise form-fitting prostheses can provide enhanced mobility and function while promoting overall comfort and wellbeing for patients with amputations, but daily activities can change the volume and temperature of the residual limb, causing potential discomfort, pressure ulcers or uneven bearing of body weight.
Now, a multi-disciplinary team of investigators led by Northwestern scientists have created a wireless, soft and flexible sensor that can constantly monitor pressure and temperature between the patient’s skin and prosthesis.
The design and development of the novel technology, detailed in a study published in Science Translational Medicine, was led by John Rogers, PhD, the Louis Simpson and Kimberly Querrey Professor of Materials Science and Engineering, Biomedical Engineering and of Neurological Surgery, and Stefania Fatone, PhD, professor of Physical Medicine and Rehabilitation.
According to Fatone, one particular challenge in prosthetics is troubleshooting the fit of prosthetic sockets, which are uniquely made to fit each patient. Fixing an ill-fitting socket typically involves receiving feedback from the patient or collecting data from traditional pressure transducers and temperature sensors that are rigid, harsh on the skin and wired to external hardware.
In comparison, the novel technology developed by Rogers’ and Fatone’s team continuously measures and monitors pressure and temperature more accurately and comfortably than conventional methods, reducing the risk of irritation and damage to the patient’s skin.
“We ended up with something that was pretty unique and different than anything that we’ve done in the past, because it’s not only flexible but can withstand very harsh environments. It was a great engineering challenge,” Rogers said.
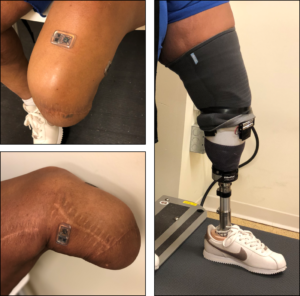
The wireless sensor, which is no larger than a postage stamp, contains a pressure sensor with a built-in temperature sensor. The sensor gently mounts to the surface of the skin of the patient’s residual limb, while a wireless data reader module is attached to the outside of the prosthetic socket.
The sensor and the module work hand-in-hand: the sensor wirelessly sends pressure and temperature data to the module, while the module wirelessly provides power to the sensor and transmits data from the sensor to a nearby smartphone or computer through Bluetooth.
Developing the technology was no simple feat, however, according to Rogers. Prosthetic sockets are a particularly challenging environment to work with, as they involve multiple layers of material varying in thickness that can interfere with data transfer and constantly apply mechanical force and stress to the sensors.
“The challenge was how do you maintain the soft, supple mechanics but in a platform that is not going to mechanically be damaged by the kinds of forces and conditions in a prosthetic socket,” Rogers said.
Ultimately, the team was able to design sensors that can withstand constant force and pressure without breaking, all the while being soft to the touch and flexible enough to gently adhere to the patient’s skin.
After developing multiple protoypes, the investigators were able to test a final version of the technology on one patient with a transtibial (below the knee) amputation and another with a transfemoral (above the knee) amputation. Overall, the technology accurately and continuously captured pressure and temperature levels without causing skin irritation or damage for both patients, according to the authors.

In the future, Fatone said the team hopes to test the device’s ability to transmit data across different patients and combinations of prosthetic materials over long periods of time.
“There’s still many challenges that we didn’t solve for, but I think the initial application is promising and has encouraged us to keep going,” Fatone said.
Rogers said the device also has potential for wider clinical and research applications that require measuring pressure and temperature, such as monitoring patients in hospital settings for bedsores or for patients that use medical compression stockings.
“We’re open to partnerships that would allow us to take this out of a purely laboratory demonstration mode into something that could be manufactured, scaled, distributed and refined as necessary to take it to the next level,” Rogers said.
Co-authors of the study included Shuai Xu, MD, ’18 GME, assistant professor of Dermatology in the Division of Translational Dermatology and Research and of Pediatrics in the Division of Dermatology; and Yonggang Huang, PhD, the Walter P. Murphy Professor of Mechanical Engineering, Civil and Environmental Engineering, and Materials Science and Engineering at the McCormick School of Engineering.
This work was supported by the Eunice Kennedy Shriver National Institute of Child Health and Human Development, the National Institute of Biomedical Imaging and Bioengineering grant R01EB019337, and the National Institute on Aging Small Business Innovation Research grant 1R43AG059445-01.






