Blocking a sodium channel decreased scarring and symptoms of atopic dermatitis, an inflammatory skin disorder, by improving the skin’s barrier function in a new Northwestern Medicine study published in Science Translational Medicine.
The skin helps keep allergens and bacteria out of the body, but perhaps its most important role is keeping water inside the body. Impaired skin barrier function and water loss is not only a characteristic of skin diseases, it also leads to delayed wound healing and abnormal scarring.
In the study, scientists focused on the regulation of sodium ions, which are crucial for maintaining the body’s balance of fluids. Sodium dysregulation is a hallmark of inflammatory skin disorders, from eczema to psoriasis.
“Maintaining sodium homeostasis has always been known to be critical for any cell or organism from bacteria to humans,” said Thomas Mustoe, MD, the study’s senior author and a health system clinician in the Department of Surgery Division of Plastic Surgery. “But the role that sodium concentration plays as an upstream regulator of important signaling pathways has not been previously described.”

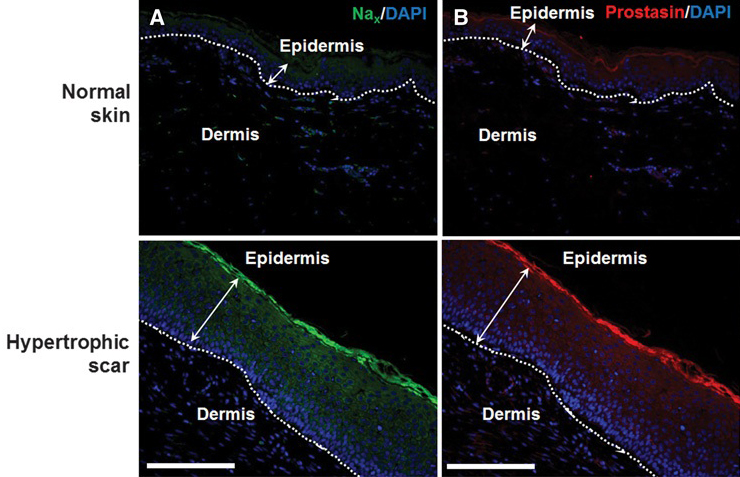
In previous research, Mustoe’s team showed that hydration helps wounds heal faster and prevents abnormal scars from developing. But when the skin barrier is compromised and there’s not enough hydration, an increased flow of sodium initiates the inflammation that can lead to skin problems. In the new study, the scientists learned that a sodium channel protein, Nax, recognizes the increased sodium concentration that occurs when the skin barrier is disrupted and induces this inflammation.
“The sodium sensor protein is a key molecule that regulates inflammation,” said co-first author Seok Jong Hong, PhD, research assistant professor of Surgery in the Division of Plastic Surgery. “Blocking the expression of Nax results in improvement in scarring and atopic dermatitis.”
The scientists used a DNA microarray analysis to identify the genetic pathway through which Nax controls inflammation. Then they developed a small interfering RNA (siRNA) that inhibited the sensor protein, thus preventing inflammation in animal models. The work suggests that Nax may be a promising therapeutic target for patients with abnormal scarring or skin disorders like eczema. It might even have the potential to improve inflammatory conditions beyond the skin.
“The wide distribution of Nax in many organs makes this channel protein potentially involved in the regulation of many cell activities through mediating sodium homeostasis,” Hong said. “Therefore, Nax is a likely candidate to regulate inflammation in other organs, such as the kidney, gastrointestinal tract and lung.”
The study was supported by the Division of Plastic and Reconstructive Surgery and the Geneva Foundation.






