Justinian University Hospital survives with no cardiac monitoring, very little oxygen, few lab tests, and three to five hours without electricity each and every day.
But even under these conditions, the second largest hospital in Haiti continues to save lives, treat patients, and help the Caribbean nation rebuild from the January 12, 2010, earthquake that claimed more than 200,000 residents.
“Haiti is not in disaster mode anymore,” said Rahul Khare, MD, assistant professor of emergency medicine at Northwestern University Feinberg School of Medicine. “When I initially came about two weeks after the earthquake, the country needed emergency care and all of the physicians were dealing with their own family members. It was truly a disaster. Two years later, all of the hospitals are run by Haitians, people are getting to see their own primary care physicians, and there is less reliance on foreign healthcare workers.”
From February 4 through 11, Khare embarked on his third trip to Haiti, this time to deliver a series of lectures on emergency medicine and to work side-by-side with Haitian doctors and medical students in the city of Cap Haitien.

A few months ago, the Israeli Ministry of Health upgraded the Justinian University Hospital with a new Critical Care Unit (CCU). As the education and operations lead, Jewish Healthcare International sent Khare and three other volunteers to gather facts and make sure the CCU is being used correctly.
“The CCU is like no other part of the hospital. When you walk in you feel this rush of cold air and cleanliness. It is the only place, other than the operating rooms, with central air conditioning,” Khare said. “There is a waiting room with two rooms next to it where a patient can be triaged, then a second door leads you to a long hallway lined with clean beds. To the left is a room that looks like our trauma/resuscitation bay at Northwestern Memorial Hospital. There’s a monitor, cart for emergent procedures, medication cart, suction, in-wall oxygen, and enough room for multiple people to work on the patient.”
Thirty seconds away sits the emergency room, where patients are initially seen by interns and are treated on a first-come, first-served basis. There is no triage and the attendings are internal medicine doctors without any emergency medicine training.
“In a word, the ER is chaotic. It is also dirty, extremely smelly, not sanitary, and because there are no supplies or nurse assignments, it’s disorganized and inefficient,” Khare said. “There are no Haitian emergency physicians, as it is a young specialty even in the U.S. How do you teach a specialty to medical students and residents if it was never taught to the faculty?”
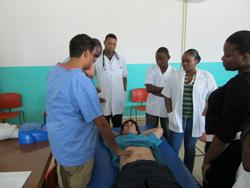
With the help of a translator, Khare began that teaching process with a series of lectures to groups of physicians and nursing students. But the night before his first talk, on acute myocardial infarction, Khare had to make major revisions. It turns out that the hospital does not have tests for cardiac biomarkers, the substances that are released into the blood when the heart is damaged or stressed.
“It was interesting to give a lecture on heart attacks without the main way we diagnose it,” he said.
Although Khare, who blogged about his trip, doesn’t have any definite plans to make a return visit to Haiti, he did hint at the distinct possibility.
“I went to Haiti initially to help with the disaster after the earthquake, but I realize now that I was so struck, and so at awe of the people, that I keep on wanting to come back,” he said. “It gets a bit harder for me to help because just giving your care to the Haitians is not necessarily a good thing for them. Educating them, showing them advances in care, and teaching new techniques such as triage and emergency care are ways to give them a lasting change that will hopefully help them for years or decades to come.”