May 19, 2004
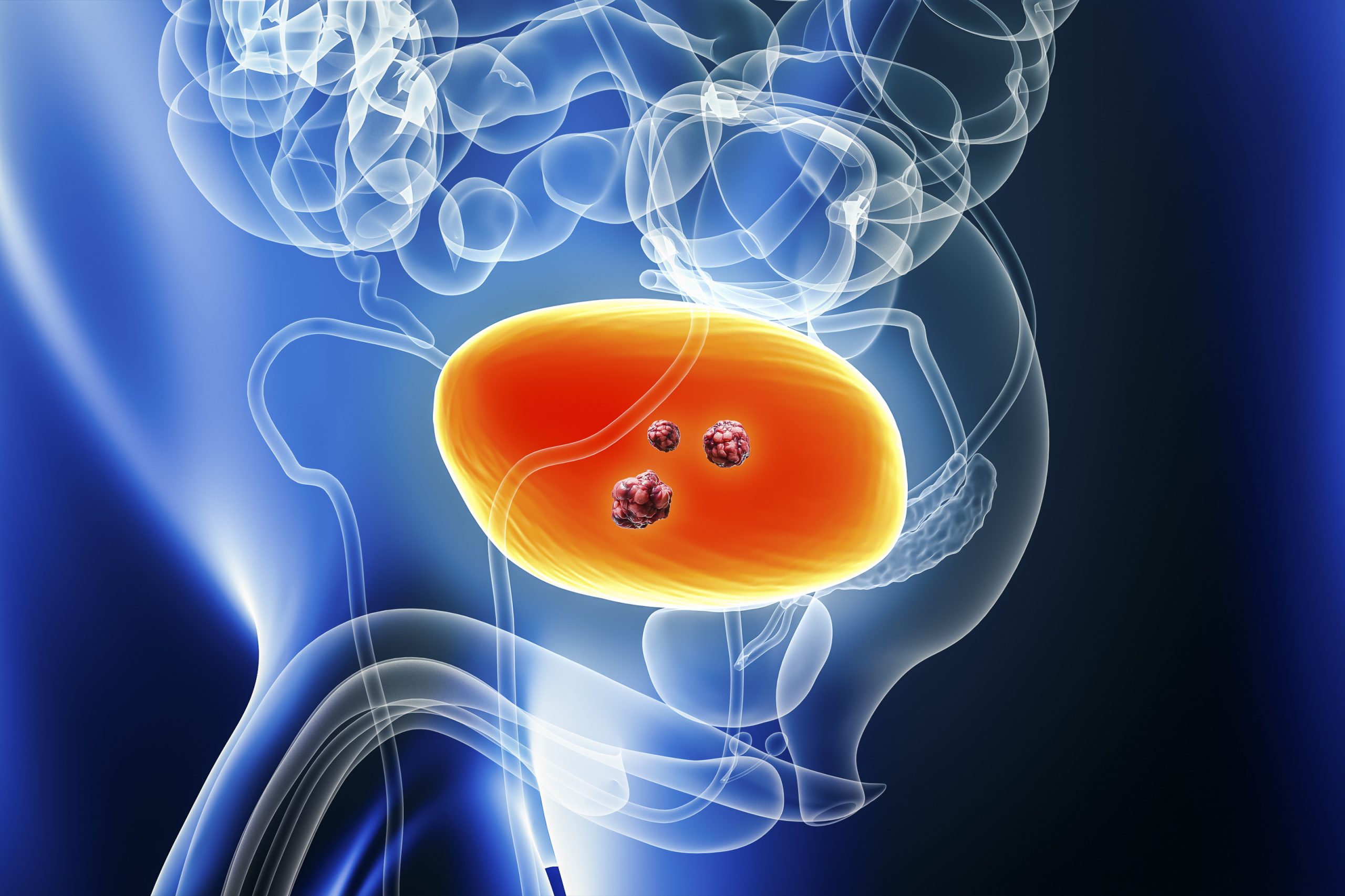
Mechanism Found That May Protect Kidneys in Early Stages of Diabetes
CHICAGO— A group of Northwestern University researchers has identified what they believe is a built-in biological mechanism that prevents kidney damage in the early stages of diabetes associated with obesity.
Their study was led by Daniel C. Batlle, MD, Earle, del Greco, Levin Professor of Nephrology and professor of medicine at Northwestern University’s Feinberg School of Medicine, and was published in the May issue of the journal Hypertension.
Dr. Batlle and colleagues assessed the activity of two enzymes, ACE (angiotensin-converting enzyme) and ACE2, which play an important role in controlling blood pressure, in the kidneys of a young mouse model of obesity and diabetes. The mouse, called db/db, develops type 2, insulin-resistant diabetes and obesity four to seven weeks after birth and eventually manifests some, but not all, features of human diabetic nephropathy.
In eight-week old db/db mice that were obese and had high levels of blood glucose but no evidence of diabetes-related kidney disease, the researchers found low levels of ACE and increased levels of the related enzyme ACE2.
The significance of a reduction in ACE coupled with increased ACE2 production in the kidneys needs to be clarified, said Minghao Ye, research associate in medicine at the Feinberg School and first author on the study.
ACE is required for production of angiotensin II (AngII), which, among its actions, causes blood vessel constriction and sodium and water retention by the kidney, leading to hypertension and kidney damage. ACE inhibitors, which block production of AngII, are commonly used to treat high blood pressure and heart failure, as well as to improve survival after a heart attack and slow progression of kidney disease in individuals with diabetes.
ACE2, which was recently discovered, prevents accumulation of AngII while promoting formation of another substance called Ang(1-7), which dilates blood vessels and helps eliminate excess water and sodium from the kidneys. ACE inhibitors do not block ACE2 production.
“Since AngII overproduction is thought to play a pivotal role in the progression of diabetic nephropathy, we suggest that decreased renal ACE activity coupled with increased renal ACE2 expression may be protective for the kidneys in the early phases of diabetes by limiting the renal accumulation of AngII and possibly favoring Ang(1-7) formation,” Dr. Batlle said.
Interestingly, the finding of a decrease in ACE activity and an increase in ACE2 expression in the young mouse model is similar to a pattern seen after administering a kidney-protecting drug and ACE inhibitor called ramipril to diabetic rats, Dr. Batlle said.
He added that an increased ACE2 level in the kidneys in early diabetes does not exclude the possibility of an ACE2 reduction later during the course of the disease as kidney damage develops. Dr. Batlle believes that with time decreased ACE2 expression accompanied by increased ACE levels may foster damage in diabetes.
“The significance of a reduction in ACE coupled with increased ACE2 production in the kidneys needs to be further studied, but there is every reason to believe that it can only be beneficial,” Dr. Batlle said. “We know that giving ACE inhibitors can protect against kidney disease, but we need to learn more about ACE2 in diabetes, obesity and hypertension,” he said.
Kidney disease is among the most common complications of diabetes, affecting more than 20 percent of the 17 million diabetic patients in the United States.
In addition to Ye, Dr. Batlle’s co-researchers on the study were Jan Wysocki, Parveen Naaz, Mohammad Reza Salabat, and Michael S. LaPointe of the Feinberg School