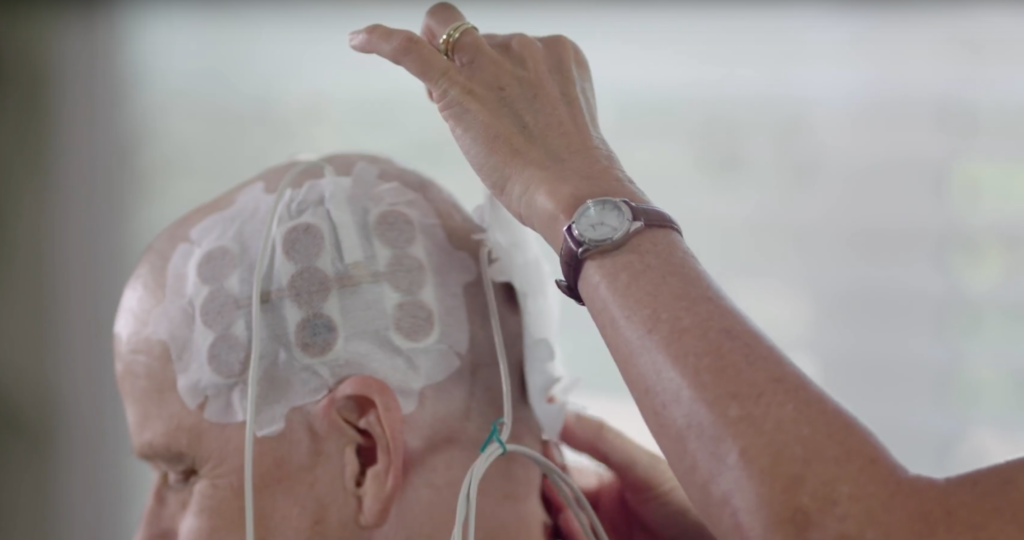
Electric fields slow growth of brain tumor in glioblastoma

A device attached to a patient’s scalp that delivers a continuous dose of low-intensity electric fields improves survival and slows the growth of a deadly brain tumor, according to a new clinical trial led by a Northwestern Medicine scientist, published in the journal JAMA.
The new treatment for glioblastoma uses alternating electric currents called tumor-treating fields (TTFields), which are delivered through an array of insulated electrodes that are affixed to a patient’s shaved scalp.
Except for occasional breaks and weekly electrode changes, patients wear the device at all times. The electrodes are connected via a cable to a small battery-powered device and continually deliver an electrical field to brain tissue.
Combining the TTFields therapy with standard maintenance chemotherapy allowed for a significant improvement in both progression-free and overall survival in patients with recently diagnosed glioblastoma.
Patients who received TTFields did better than patients who did not: the median survival time for those receiving the TTFields therapy was 20.9 months versus 16.0 months for patients who did not, with a substantially higher fraction of patients alive at two, three or four years after diagnosis.
“This trial establishes a new treatment paradigm that substantially improves the outcome in patients with glioblastoma, and which may have applications in many other forms of cancer,” said lead study author Roger Stupp, MD, chief of Neuro-oncology in the Department of Neurology.
“With TTFields therapy combined with radiation and temozolomide chemotherapy, up to 43 percent of glioblastoma patients will survive longer than two years,” said Stupp, also director for strategic initiatives at the Robert H. Lurie Comprehensive Cancer Center of Northwestern University. “In a disease where, until 2004, the great majority of patients died within one year, this is yet another example how systematic and interdisciplinary research will benefit patients in everyday care.”
Previous studies demonstrated that TTFields inhibit tumor growth and selectively affect dividing cells, ultimately leading to cancer cell death and tumor growth inhibition.
In the study, 695 patients were randomly assigned to either receive the TTFields in combination with temozolomide, a chemotherapy drug, or the chemotherapy drug alone. Overall, 466 patients received the TTFields-chemotherapy combination, and 229 received the chemotherapy treatment alone.
There was no difference in the rate of adverse events between the two groups, except for mild to moderate skin irritation on the scalp, which was experienced by slightly more than half of patients receiving the TTFields therapy.
Stupp is also a professor of Neurological Surgery, and of Medicine in the Division of Hematology and Oncology, a neuro-oncologist at Northwestern Memorial Hospital and co-director of the Lou and Jean Malnati Brain Tumor Institute at Northwestern Medicine.
The Lou and Jean Malnati Brain Tumor Institute at Northwestern Medicine helps advance medical education, collaborates on research initiatives and creates innovative clinical models of care for patients with brain and spinal cord tumors. It is a nationally recognized leader in the fight against brain and spinal cord tumors, offering patients advanced clinical trials and treatment options.
The Lurie Cancer Center supports care for a broad range of cancer types thanks to its dedication to comprehensive research, a distinguished and dedicated faculty and staff, a world-class teaching program and its commitment to making ongoing advances in medical, surgical, radiation and interventional oncology. The National Cancer Institute has designated Lurie Cancer Center as one of only 49 Comprehensive Cancer Centers in the nation recognized for their “scientific leadership, resources, and the depth and breadth of their research.”
Stupp collaborated with an international team of investigators from 83 medical centers in North America, Europe, the Republic of Korea and Israel. The TTFields device used in the study is marketed as Optune by its manufacturer Novocure, Inc., which funded the study.
Stupp received travel support from Novocure, and other authors received consulting fees, honoraria, grant support or personal fees from Novocure and from other industry research partners.






