Simulation Study Reaps Positive Results
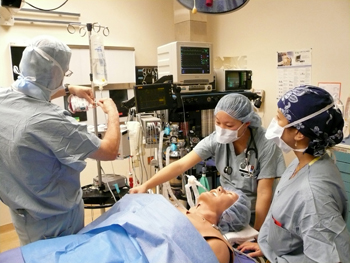 |
| Dr. Park (right) supervises anesthesiology resident Jennifer Song, MD (center) as she addresses the computer-operated needs of the patient simulator nicknamed “Cosmo.” |
Cosmo is having chest pains and trouble breathing. The anesthesiology residents leap into action. As an organized team, they listen to his breathing, monitor his falling blood pressure, send labs, and give him oxygen. Cosmo is slipping into unconsciousness. They shock his heart out of an unstable rhythm and intubate him.
Not to worry. Cosmo is a computer-operated mannequin lying in an operating room and adjoining classroom tucked off the patient waiting area on the fifth floor of the Galter Pavilion. Christine S. Park, MD, assistant professor of anesthesiology and medical director for the Patient Safety Simulation Center, is watching the intense drill on the other side of the one-way glass and studying six monitors that zoom in on the students’ work.
She and the staff have chosen a series of scenarios to train the residents to react to different critical care situations. Cosmo tells residents what his symptoms are, and if they are getting worse. Eye controls, breathing sounds, and pulse are all programmed into the mannequin. By the end of the drill, Cosmo is breathing easier. Still, just to be on the safe side, he’s heading to the intensive care unit.
The videotape of the simulation exercise will be played to the entire class of residents and the results dissected, a task critical to the process of observing and correcting clinical behaviors, says Dr. Park. Northwestern Memorial Hospital’s nurses also are tested in the center as part of their annual review, as are residents from other specialties. Fourth-year critical care students learn via high-fidelity simulation.
The simulation lab is especially important to anesthesia residents, who spend a year interning in either internal medicine or surgery, but get little exposure to an operating room or real experience providing an anesthetic. This kind of course gives them the troubleshooting skills they need when they go from intense supervision by the attending physician to acting semi-independently. The simulation scenarios are designed to prepare and then assess residents’ competence and safety when treating patients who experience low oxygen or low blood pressure.
A study conducted by Dr. Park, recipient of the Augusta Webster Grant for Educational Innovation at the Feinberg School, shows the simulation class is reaping positive results. Her research, presented at the American Society of Anesthesiologists annual meeting in Orlando, studied 21 first-year anesthesia residents as they were tested on simulation scenarios at the beginning and end of their six weeks of training. All the residents improved their performance in treating the mechanical patient’s oxygen and blood pressure events.
“The results show that the residents improved their competence in safe practice earlier than what was achieved by clinical exposure alone,” says Dr. Park. “It’s really all about patient safety. With the help of simulation, we can correct any learned action before the resident interacts with real patients.”
“We see a marked improvement and the students rave about the simulation center,” adds Dr. Park. “It helps them feel more confident—and now we have the data to back up that perception.”






